Test Prisilla again
eCPR Webinar
Webinar: COVID Variants and Vaccine Update, Mar 2, 2021
Who is eligible for this program?
Only patients who meet the indigent definition and meet the trauma criteria who are unable to pay for services and for whom there is no third-party coverage in part or in whole for trauma services provided qualify under this funding program. No reimbursement shall be provided for patient care if the patient has the ability to pay for the service but refuses or fails to pay for it.
When can I bill the program?
To bill County, Contractor must at a minimum show that it has made reasonable efforts to secure payment for the patient by billing (at least monthly) for an additional period of not less than two (2) months after the date Contractor first billed the patient.
REFERENCE: EXHIBIT B PAGE 2
What documents do I have to submit to bill the program?
- A completedOriginalUB-04 form
- A completedOriginalTSCE form (Attachment U-1)
or
- AcompletedOriginal Inability to Cooperate form (Attachment U-2)
- A printout of the data in the Trauma and Emergency Information System(TEMIS)
Hospitals must ensure that all data elements from UB-04 match the data elements from TEMIS. Claims eligible for inclusion in the County’s payment methodology shall only include claims for which all required documentation matches TEMIS.
When can an Inability to Cooperate Form (U-2) be submitted?
If a TSCE Agreement form cannot be secured because the patient is unable to cooperate in providing the necessary financial information, then a Contractor certification to that effect (Attachment U-2), Hospital Certification of Inability to Cooperate form must be completed.
Examples include, but are not necessarily limited to, situations where the patient has expired, or is comatose or otherwise, mentally incompetent.
What is the difference between Cash/Self and CHIP Eligible?
There is no difference as far as reimbursement goes. They are defined in the Trauma Data
Dictionary as follows:Cash/Self: Individuals who are not insured and do not qualify for other funding source based on ability to pay in accordance with the hospital’s charity care policy, as determined by the hospital’s finance department. For County facilities this includes ATP (Ability to Pay).
Chip Eligible: Individuals who qualify for California Healthcare for Indigents Program which provides limited funds to compensate for patients who cannot afford to pay for services rendered and for whom payment will not be made through any private coverage or by any program funded in whole or in part by the State or Federal government including Medi-Cal or Victims of Crime.
Some Trauma Centers use both they enter either CHIP or Cash as the first payer, or use only Cash and some use only CHIP. Claims submitted are reimbursed if TEMIS has either CASH/Self or CHIP Eligible in any combination. Technically, all patients for whom claims are submitted should have CHIP Eligible as either the first or 2nd payer, but as long as no other payer is in TEMIS, the County will pay.
What are the policies on refunding the County if the hospital receives payment from a patient or third party payer for claims previously paid by the County?
Any and all payments received by the Contractor must immediately be reported and the County’s payment must be refunded. Each refund should have a Trauma Hospital Payment Refund Form (Attachment B-6) attached.
REFERENCE: EXHIBIT B PAGE 8
What if the hospital has submitted a claim and payment has not been issued by the County, but Contractor is informed that there is Third Party Liability (TPL)?
Contractor must pursue the TPL and withdraw the claim by notifying the County indicating that there is pending TPL to the EMS Agency Reimbursement Coordinator at (562) 347-1590.
REFERENCE: EXHIBIT B PAGES 8 & 9
Should the hospital continue to pursue third party payer coverage once the claim has been submitted to the County for reimbursement?
No, the Contractor shall only submit claims that they have determined do not have any other payor source and the patient is indigent. If after the claims is submitted the Contractor finds out the patient does have insurance coverage, the Contractor shall notify the County and refer the payor to the County as the Contractor subrogates all their rights to the claim once they submit the claim.
What are the procedures if a provider is contacted by a third party representative (e.g., insurance claim adjuster) or a patient’s attorney regarding pending litigation for a previously submitted claim?
Contractor shall indicate that the claim for services provided to their client is assigned and subrogated to the County and refer such representatives to the designated County contact. (Contractor shall reasonably cooperate with County in its collection efforts).
What rates would the Contractor be paid if patient is admitted (i.e. on June 29th and discharged on July 5th)?
This claim would be part of the fiscal year that ended in June. Payment by County to Contractor for such patients shall be at the rates in effect on the date.
Can a claim be submitted if there is pending third party liability?
Yes, but these claims should not be submitted until the December 31st deadline nears. These claims may not be paid but will be counted towards the Medi-Cal match total.
Who is considered the last resort of payment, the County or Victims of Crime (VOC)?
A victim of Crime is considered the last resort of payment.
REFERENCE: ATTACHED VOC LETTER
Can a provider bill Victims of Crimes Program (VCP) and submit the claim to the Trauma Reimbursement Program?
No, at any point during the claiming period, the hospital has a choice of the following:
- Submit the claim to VCP and DO NOT SUBMIT to the County or
- Submit the claim to the County andDO NOT SUBMIT TO VCP
If the claim is submitted to the County and then a hospital receives payment from VCP the hospital must surrender the payment from VCP to the County.
What if a payment is received from a third party payer and they are offering less than what the County reimbursed? Can I refuse to take their payment?
No. You must immediately notify the County and refund the County’s payment.
Are in-custody patients covered by this program?
Since In-Custody claims are paid at a low rate, additional funding will be included from the Under–insured bucket when payment is issued to the trauma centers for In-Custody Claims.
1.What are the procedures if payment is received for In-Custody Claims?
- Do not submit claim if payment is received for In-Custody Claim
- Update the TEMIS database to indicate Payor 1 as In-Custody.
- TEMIS will capture the data for claims considered In Custody.
2.What are the procedures if no-payment is received on In-Custody claims?
- Submit claim if payment is not received for In-Custody Claim
- Include a copy of the denial letter from law enforcement or
- The patient notes which indicate the reason why the claim was denied.
- The TEMIS database should indicate Payor 1 as County Indigent.
What is the basis for number of hospital days reimbursed?
The number of hospital days paid will be based upon the number of hospital day room charges on the UB-92, but shall not exceed the number of days calculated between admission and discharge dates. Claims which include hospital day room charges on the UB-92 that exceed the calculated number of days between hospital admission and discharge will be returned for correction.ing hospitalization, they are not eligible. (The key is the status while hospitalized).
Zika Virus — June 15, 2016
Zika virus is a flavivirus spread by the bite of the Aedes mosquito and is related to denque, yellow fever and West Nile viruses.
Originally reported in Uganda, the virus has now spread to many parts of the world including the United States (See Figures).
http://www.cdc.gov/zika/geo/active-countries.html
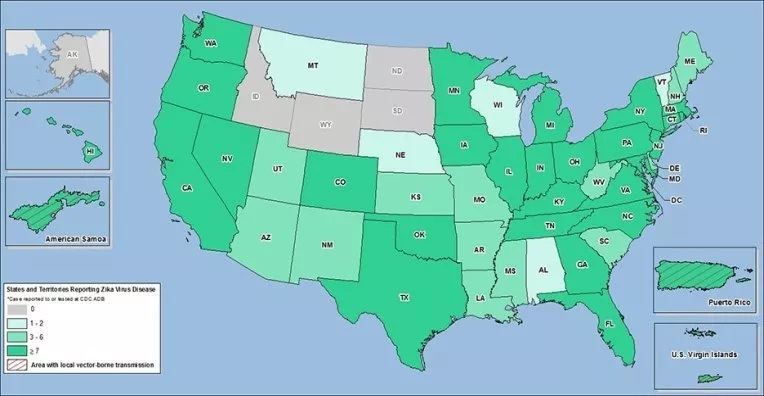
Incubation is 2-12 days and only 20% of patients bitten develop symptoms. Transmission between humans can occur via blood transfusion or sexual activity. Symptoms include fever, rash, conjunctivitis, joint pain, headache, and generalized weakness.
One of the most publicized complications is microcephaly in babies born of women infected with the virus during pregnancy (generally in the first trimester of pregnancy). Greater than 4000 cases have been reported in Brazil and now in other areas of the world.
Treatment of the disease is symptomatic meaning treating the fever and symptoms with acetaminophen (Tylenol) and other supportive care such as IV fluids if dehydrated. Ibuprofen (Motrin) should be avoided as co-infections with dengue do occur and use of nonsteroidal anti-inflammatory agents, such as ibuprofen, may increase risk of progression to hemorrhagic fever.
Testing for the virus can occur from blood, urine or cerebrospinal fluid specimens sent to local health departments. http://www.cdc.gov/zika/hc-providers/index.html
EMS providers should use universal precautions or standard infectious disease precautions (gloves and mask) when evaluating and transporting these patients to the emergency department. Exposure to blood or bodily fluids should be reported per normal guidelines and no additional precautions are necessary. Questions regarding exposures can first be directed to the Medical Alert Center who can contact Public Health.
Reference:
- United States Center for Disease Control and Prevention http://www.cdc.gov/zika accessed 7-11-16.
- Los Angeles County Department of Public Health http://publichealth.lacounty.gov/acd/vectorzika.htm accessed 7-11-16.
- Los Angeles County Department of Public Heath http://publichealth.lacounty.gov/acd/docs/ZikaCDRoundsMay201
The End of Life (AB15) Impacts on EMS System — June 20, 2016
TO: The EMS Community
As many of you are aware, in late 2015, the California Legislature passed the End of Life Act (AB 15), which became law on June 9, 2016. This Act allows for terminally ill patients in California who are mentally competent adults to voluntarily request and receive a prescription for medication to end the patient’s life at a time of their choosing. This allows for a patient to have some control over the end of their life and gives patients dignity and comfort at the time of their death.
The law outlines many safeguards for the patient and includes language that the patient may rescind his/her wish to take the aid-in-dying drug at any time.
In order to prepare the EMS system to care for these patients with respect for their wishes, there have been modifications to a number of key EMS Agency policies including Reference No. 814 “Determination/Pronouncement of Death in the Field” and Reference No. 815 “Honoring Do Not Resuscitate Orders”, Physician Orders for Life Sustaining Treatment, and the End-of-Life Option (Aid-in-Dying drug).
Please review these updated policies on our website under Resources/Prehospital Care Manual. Note a couple of new resources within Reference No. 815: Reference No. 815.3 provides an example of an attestation that the patient intends to take the Aid-in- Dying Drug within 48 hours. An attestation may or may not be available at the time EMS arrives at a home of a patient who has taken the aid-in-dying drug. Reference No. 815.4 is an algorithm, which is intended to provide guidance on the management of these patients. The goal is to honor a patient’s end-of-life option and provide comfort and guidance to the family.
We must also work collaboratively as EMS and hospital-based providers to make the best decisions on care and transport for the patient, and their families.
Sincerely,
Marianne Gausche-Hill, MD, FACEP, FAAP
Medical Director, LA County EMS Agency
Links:
Reference No. 814, Determination/Pronouncement of Death in the Field
Reference No. 815.4, End of Life Options Field Quick Reference Guide
Paramedic to Assist caregivers or patient with self-administered emergency medication
In this update I will:
- Discuss the authority for paramedics to administer emergency medication including hydrocortisone for patients with congenital adrenal hyperplasia (CAH).
- Define adrenal crisis and its causes
- List signs and symptoms of adrenal crisis
- Describe the appropriate field treatment for a CAH patient in the prehospital setting
Congenital adrenal hyperplasia or CAH are any of several types of genetic diseases (autosomal recessive) that can result in excessive or deficient production of sex steroids or cortisol. This can have a profound effect on the reactions of the body to stress including infection.
- The adrenal glands sit on top of both kidneys and produces hormones including cortisol, aldosterone, and testosterone.
Adrenal crisis is a life-threatening condition that occurs when there is not enough cortisol produced. - Congenital adrenal hyperplasia (CAH) is an autosomal recessive genetic disorder which results in improper hormone synthesis resulting in, with stress such as an infection, adrenal crisis.
- Causes of adrenal crisis include deficiency anywhere along the pathway to cortisol production and release by the adrenal glands. CAH is one cause. Patients with dysfunction of the adrenal glands themselves (known as Addison’s disease), and those with disease of the pituitary may also have adrenal crisis with stressors.
Any of the following stresses to the normal physiology of a patient with CAH or other diseases of the adrenal gland can result in life threatening consequences:
Infection
Physical Stress
Dehydration
Surgery
Sudden discontinuation of medication
Injury to the pituitary or adrenal gland
Signs and symptoms are not specific for adrenal crisis, so a high level of suspicion for this condition should be maintained for a patient with CAH. These signs and symptoms may include:
- Nausea
- Fever
- Pallor
- Confusion
- Weakness
- Tachycardia
- Tachypnea
- Hypotension/shock
IF LEFT UNTREATED CAN RESULT IN DEATH
CASE ILLUSTRATON
Let’s illustrate what we are discussing by presenting a case:
Paramedics respond to the home of a 2 year-old boy
Teenage sister states the boy began to have fever, vomiting and diarrhea several hours ago
She states the child has congenital adrenal hyperplasia
He is wearing a medical alert bracelet that states “adrenal insufficiency”
The boy’s vital signs:
HR 180, RR-30,
Cap refill-delayed 3 secs
LOC- Responds to verbal by moving head and crying
Skins- Hot to touch
Sister states she tried to give the child a double dose (stress dose) of hydrocortisone (Solu-Cortef®) by mouth as prescribed by the physician, but the child immediately vomited it up.
She attempted to contact her parents but they did not answer her phone call.
Her mother usually gives him an IM injection of hydrocortisone (Solu-Cortef®) when he cannot tolerate medication by mouth.
She has his injection kit next to her.
What should the paramedic do?
What can the paramedics do?
Per State of California Title 22, Division 9, Prehospital Emergency Medical Services, Chapter 2, EMT 100063: Scope of Practice of EMT Assist patients with the administration of physician prescribed devices including but not limited to, patient operated medication pumps, sublingual nitroglycerin, and self-administered emergency medications, including epinephrine devices
Paramedics may perform any activity in the scope of practice of an EMT, therefore can assist patients in delivering normally self-administered medications, such as hydrocortisone in this case (other examples of emergency self-administered medications include albuterol, nitroglycerin, or epinephrine via autoinjector)
In summary
- If a patient has CAH has symptoms of adrenal crisis, the EMT or paramedic can assist the patient, or patient’s caregivers in administering the medication (hydrocortisone (Solu-Cortef®) IM) which falls under both EMT and paramedic scope of practice
- A paramedic should contact the base hospital with any questions
- These patients must be transported to the hospital for further evaluation/treatment
- This medication should be given as soon as possible and can be life saving
Please see attached Presentation for further information
Hepatitis A Outbreak in Los Angeles County — September 21, 2017
The Los Angeles County Department of Public Health has notified the Emergency Medical Services (EMS) Agency of 10 cases of Hepatitis A amongst our homeless population or others at risk for Hepatitis A infections.
In San Diego County 421 cases of Hepatitis A infections including 16 deaths, primarily affecting homeless persons, injection and non-injection illicit drug users and individuals in dense living conditions with shared restrooms, were reported since November 2016.
At this time we recommend that all EMS Provider Agencies and Police Departments notify their staff who have direct contact with individuals from the identified population, of this outbreak and the need for vigilance relative to PPE use and hand hygiene. Although hand hygiene should be a part of daily clinical care both for the protection of the provider and the patient/client, outbreaks such as these bring this practice into the forefront of prehospital care. Hepatitis A virus is spread by oral contamination with feces which occurs when a person puts their contaminated hand in their mouth. This transmission can be prevented by PPE and good hand hygiene practices. These same practices are important for law enforcement personnel to follow to prevent exposure to disease.
The Center for Disease Control (CDC) recommends the following best practice related to hand hygiene and use of gloves for health care providers:
When and How to Wear Gloves
- Wearing gloves is not a substitute for hand hygiene. Dirty gloves can soil hands.
- Always clean your hands after removing gloves.
- Steps for Glove Use:
- Choose the right size and type of gloves for the task
- Put on gloves before touching a patient’s non-intact skin, open wounds or mucous membranes, such as the mouth, nose, and eyes
- Change gloves during patient care if the hands will move from a contaminated body-site (e.g., perineal area) to a clean body-site (e.g., face)
- Remove gloves after contact with a patient and/or the surrounding environment (including medical equipment) using proper technique to prevent hand contamination
- Failure to remove gloves after caring for a patient may lead to the spread of potentially deadly germs from one patient to another
- Do not wear the same pair of gloves for the care of more than one patient
When Should an EMS providers and Law Enforcement Personnel Use Alcohol Based Sanitizers or Wash Hands
- Before eating
- Before and after having direct contact with a patient’s intact skin (taking a pulse or blood pressure, performing physical examinations, lifting the patient in bed)
- After contact with blood, body fluids or excretions, mucous membranes, non-intact skin, or wound dressings
- After contact with inanimate objects (including medical equipment) in the immediate vicinity of the patient
- If hands will be moving from a contaminated-body site to a clean-body site during patient care
- After glove removal
- After using a restroom
When using alcohol-based hand sanitizer:
- Put product on hands and rub hands together
- Cover all surfaces until hands feel dry
- This should take around 20 seconds
Each EMS Provider Agency should alert their providers to the CDC recommendations on who should be vaccinated against Hepatitis A.
Currently the Hepatitis A Vaccine is recommended for the following persons aged 1 year and older:
- Persons who live/work in a community with a high rate of Hepatitis A (HAV)
- For men having sex with other men.
- For drug users.
- Travelers to countries with high rates of Hepatitis A.
- Persons with chronic liver disease.
- Persons who receive blood products to help your blood clot (e.g. Hemophilia).
- Persons working with HAV-infected animals or work with HAV in research setting.
The Hepatitis A vaccine is currently given to all children after 1 year of age – this occurred after 2000 – thus many of our EMS providers and law enforcement personnel may be unvaccinated. The Hepatitis A vaccine is given in two injections 6 months apart and confers 25 year immunity in most adults.
For the latest updates and recommendations please visit the EMS Agency website at:
Under Important Notice on the landing page is an area listed as Hepatitis A Update. You can click on this to be linked to the most current information from the Department of Public Health. If you have specific questions please send them to HepAinfo@dhs.lacounty.gov and EMS Agency staff will get back to you with a response.
* Updates
* Message from the Medical Director — October 6, 2017
Seasonal Infuenza — January 8, 2018
Fentanyl Exposure for EMS Provider — August 30, 2018
Fentanyl use as a drug of abuse has increased in the United States. EMS providers are increasingly likely to encounter fentanyl in the line of duty.
Facts to know:
- Fentanyl is a synthetic opioid that is more potent than heroin or morphine
- Fentanyl can be present in many forms (e.g. tablet, capsule, powder, rocks, solutions)
- Inhalation of fentanyl as an airborne powder is the most likely exposure route that would lead to harmful effects, but it is less likely to occur than skin contact.
- Incidental skin contact is not expected to lead to harmful effects if the contaminated skin is promptly washed off with soap and water.
Signs and symptoms of fentanyl exposure include:
- Respiratory Depression
- Drowsiness or Unresponsiveness
- Constricted or Pinpoint Pupils
Prevention:
- PPE is effective in decreasing the risk of harmful effects from fentanyl exposure
- Wear gloves to prevent skin exposure
- NIOSH-approved respirators (“masks”) decrease the risk of inhalation exposure
- Eye protection can prevent mucous membrane exposure
If exposure occurs:
- Do not touch your eyes, mouth, nose or any skin after touching a potentially contaminated surface
- Wash skin thoroughly with soap and water; Do NOT use hand sanitizers as they may enhance absorption through the skin
- If you suspect clothing contamination, remove them via standard decontamination procedures
If an EMS responder exhibits signs or symptoms of fentanyl exposure:
- Move away from the source and call for assistance
- Administer naloxone per departmental protocols
- Perform rescue breathing/airway management as needed
- Administer CPR if indicated
US Customs and Border Protection: https://www.youtube.com/watch?v=6Yc9lSaSKls
Safety Recommendations for First Responders Handout: https://www.whitehouse.gov/sites/whitehouse.gov/files/images/Final%20STANDARD%20size%20of%20Fentanyl%20Safety%20Recommendations%20for%20First%20Respond….pdf
Flea-Borne Typhus? — October 18, 2018
Los Angeles County Department of Public Health (LAC DPH) has identified a number of cases of flea-borne typhus associated with the homeless population in downtown Los Angeles and the Willowbrook area of Compton.
LAC DPH states, “flea-borne typhus, also known as murine or endemic typhus, is a disease transmitted by fleas infected with Rickettsia typhi or Rickettsia felis. Flea-borne typhus is endemic in LAC with cases detected each year. In recent years, the average number of cases reported to LAC DPH has doubled to nearly 60 cases per year; however, geographic clusters of the size are unusual. Most cases occur in the summer and fall months. In LAC, the primary animals known to carry infected fleas include rats, feral cats, and opossums. People with significant exposure to these animals are at risk of acquiring flea-borne typhus”
When should EMS providers suspect typhus?
- A fever of unknown cause, especially in patients at high risk (e.g., homeless, or those around feral cats or other mammals).
- Other symptoms include chills, body aches, headache, and rash.
What are recommended actions by emergency departments and other hospital-based clinicians?
Consider a diagnosis of flea-borne typhus in patients with a non-specific febrile illness with headache, myalgia, rash, and laboratory abnormalities including leukopenia, thrombocytopenia, and elevation of hepatic transaminases, without alternate identifiable etiology.
- LAC DPH asks that all suspected cases of flea-borne typhus, particularly in persons experiencing homelessness and those with exposure to outdoor animals such as stray cats, opossums, pet dogs and cats, be reported to Los Angeles County DPH Acute Communicable Disease Control Program within 1 working day.
- Weekdays 8:30 AM – 5:00 PM: call 888-397-3993. For consultation: call 213-240-7941
– After hours: call 213-974-1234, and ask for the physician on call.
Long Beach Health and Human Services
- Weekdays 8:00 AM – 5:00 PM: call 562-570-4302
– After hours: call 213-974-1234, and ask for the physician on call.
Pasadena Public Health Department
-
- Weekdays 8:00 AM – 5:00 PM (closed every other Friday): call the Communicable Disease Control Program at 626-744-6089
– After hours: call 626-744-6043.
- Weekdays 8:00 AM – 5:00 PM (closed every other Friday): call the Communicable Disease Control Program at 626-744-6089
- LAC DPH recommends that treatment for typhus not be delayed for diagnostic testing which includes serologic testing for R.typhi IgG and IgM antibodies. As there can be cross-reactivity with other rickettsiae, LAC DPH also recommends testing for antibodies against R. rickettsii, the causative agent of Rocky Mountain Spotted Fever. http://www.publichealth.lacounty.gov/acd/TyphusTesting.htm
- Doxycycline is the treatment of choice; the dose of doxycycline for adults is 100 mg orally BID. Treatment should occur for a minimum of five days or until 48 hours after patient becomes afebrile.
Are there concerns about contracting the disease if EMS or hospital personnel care for such patients?
- There is no concern for person-to-person transmission therefore, standard precautions and PPE are indicated.
- No additional methods for cleaning of ambulances after transport of suspected patients are indicated.
If fleas are noted, consider removing clothing and place in a biohazard bag.
Additional Resources
- Los Angeles County Department of Public Health Flea-borne Typhus webpage
www.publichealth.lacounty.gov/acd/VectorTyphus.htm
- California Department of Public Health Flea-borne Typhus webpage
www.cdph.ca.gov/Programs/CID/DCDC/Pages/Typhus.aspx
- Centers for Disease Control and Prevention Murine Typhus webpage
www.cdc.gov/typhus/murine/
COVID-19 Outbreak: An Update
http://publichealth.lacounty.gov/acd/nCorona2019.htm
https://www.cdc.gov/coronavirus/2019-ncov/hcp/guidance-for-ems.html
https://www.cdc.gov/coronavirus/2019-nCoV/
The CDC does have an emergency operations center if there is additional information needed and that’s at (770) 488-7100.
Where else can I get reliable information about COVID-19?
Below is a list of resources that can provide reliable information about COVID-19:
Should SNFs or receiving hospitals screen EMS providers upon arrival?
The Los Angeles County EMS Agency recommends against SNFs screening EMS providers because every EMS provider is screened by their employer regularly and performs self-monitoring. Extra screening provides no benefit, and may delay patient care.
What personal protective equipment (PPE) should I don prior to entry to a SNF?
Proper PPE for entering a SNF includes a surgical mask, eye protection, and gloves. For any call with aerosol generating procedures an N95 should be donned, and a gown if supplies allow.
What is the Los Angeles Surge Hospital (LASH)?
The Los Angeles Surge Hospital (LASH) is a surge hospital that was opened in response to the COVID-19 pandemic in order to decompress other hospitals and to create more hospital beds within Los Angeles County. The LASH is accepting COVID-19 positive patients only. The LASH accepts patients through interfacility transports only and is not a designated 9-1-1 receiving facility.
What are I/Q sites and should I be responding any differently to them? How can I refer a patient to the I/Q sites?
I/Q sites are “isolation and quarantine” sites that have been set up around the county to safely house COVID-19 test positive patients, suspected COVID-19 patients, or patients under quarantine isolation due to an exposure. Responding to this site should be no different than the standard response, as you should be responding to all calls with a surgical mask, gloves, and eye protection at the minimum. These sites have nursing and medical staff on site that may be able to provide you with more information about the patient. Medical equipment on site is severely limited.
In order to refer a patient to the I/Q sites, a Public Health community volunteer may be contacted and to screen and determine if the patient qualifies for the I/Q sites. A community worker list is available on our website. EMS is not required to make this referral.
What is the Fairview ACS Transfer Package?
Fairvew ACS Transfer Package
Where can I find more information on applying for approval to transport medical patients to an alternate destination during the COVID-19 pandemic?
Are EMS personnel authorized to transport patients to alternate destinations?
Transport to alternate destinations that are not located on a 9-1-1 Receiving Facility campus is not authorized unless your Provider Agency is participating in an approved pilot program. EMS personnel may be directed by the 9-1-1 receiving facility to an alternate triage/care site ON campus and adjacent to the Emergency Department, such as a triage tent. The 9-1-1- Receiving Facility is required to submit a plan to the LA County EMS Agency and to the Provider Agencies in the region. See COVID-19 Update # 8 for more information.
What are alternate destinations?
Should receiving hospitals screen EMS providers upon arrival?
When should I doff my PPE?
What should I do if I am performing an aerosol generating procedure (AGP) upon arrival to the receiving facility?
For patients resuscitated from cardiac arrest, why am I staying on scene to stabilize the patient after return of spontaneous circulation (ROSC)?
For patients without return of spontaneous circulation (ROSC), why am I consulting with the Base Physician regarding the decision to transport?
How does treat and refer work? What if the patient still wants transport?
If the patient or legal guardian still requests transport after reassurance by EMS personnel, then the patient must be taken to the Most Accessible Receiving facility (MAR) for adults or Emergency Department Approved for Pediatrics (EDAP) for children
If there is a disagreement between TP 1245 and the treatment protocol corresponding with the provider impression, which protocol should be followed?
Is there a treatment protocol for COVID-19 patients?
Where can I find more information on applying for waivers for prehospital care policies during a disaster/emergency declaration?
What are aerosol generating procedures (AGPs)?
Can we reuse PPE between patients/calls?
What is the appropriate level of PPE to wear on calls?
If I test positive for COVID-19, when can I go back to work?
Where can I get tested for COVID-19?
What is active monitoring?
This differs from self-monitoring where all on-duty EMS providers monitor themselves for fever by taking their temperature twice a day and monitor for symptoms of COVID-19. See CDC’s guidance on monitoring and LA County EMS Agency’s Guidance for more information.
What is considered a high-risk exposure and what should I do if I have experienced one?