MD01
CASE OF THE MONTH – OCTOBER 2022
Case Presentation:
 EMS responds to the medical treatment area of a large outdoor festival venue for a 21-year-old female who, according to medical providers on scene, was found unconscious by friends about 15 minutes prior. The patient’s friends state she had been drinking alcohol, smoking marijuana and “may have used some other stuff,” but they hesitate and say that they are not sure what. The medical staff found her cyanotic with poor respiratory effort and gave Narcan 2mg IN with minimal improvement.
EMS responds to the medical treatment area of a large outdoor festival venue for a 21-year-old female who, according to medical providers on scene, was found unconscious by friends about 15 minutes prior. The patient’s friends state she had been drinking alcohol, smoking marijuana and “may have used some other stuff,” but they hesitate and say that they are not sure what. The medical staff found her cyanotic with poor respiratory effort and gave Narcan 2mg IN with minimal improvement.
Her initial vital signs are BP 110/80, HR 124, RR 10, SpO2 83% on room air, 86% on 15L via BMV
In addition to her altered level of consciousness, she is tachycardic and hypoxic. These abnormalities should drive immediate management. For specific treatment, there are several provider impressions to consider, including Overdose/Poisoning/Ingestion, Respiratory Distress-Other (pulmonary embolism, pneumothorax), Respiratory Distress-Bronchospasm, Traumatic Injury, or a first-time presentation of an undiagnosed medical condition such as a cardiac or renal problem.
In the context of the patient being otherwise healthy at a concert event where drugs of abuse are commonly encountered, ingestion or intoxication should be strongly considered. Given that this patient is presenting with an altered level of consciousness, a full assessment is critical prior to determining the most suitable provider impression.
Initially, TP-1229 Altered Level of Consciousness (ALOC) should be used in conjunction with TP-1241, Overdose/Poisoning/Ingestion to guide management.
On further assessment, the patient’s GCS is 1-2-5 (8). Her pupils are normal in size and reactive. She has good chest rise with bag mask ventilations and an EtCO2 of 33. Her lungs are clear on auscultation without wheezing or rhonchi. There are no external signs of trauma on exam. Her blood glucose is 125mg/dL. Capillary refill is poor, and her hands appear cyanotic. Her ECG shows sinus tachycardia without ST-segment elevation.
When you place an IV, you notice that her blood looks unusually dark. It is a deep chocolate brown.
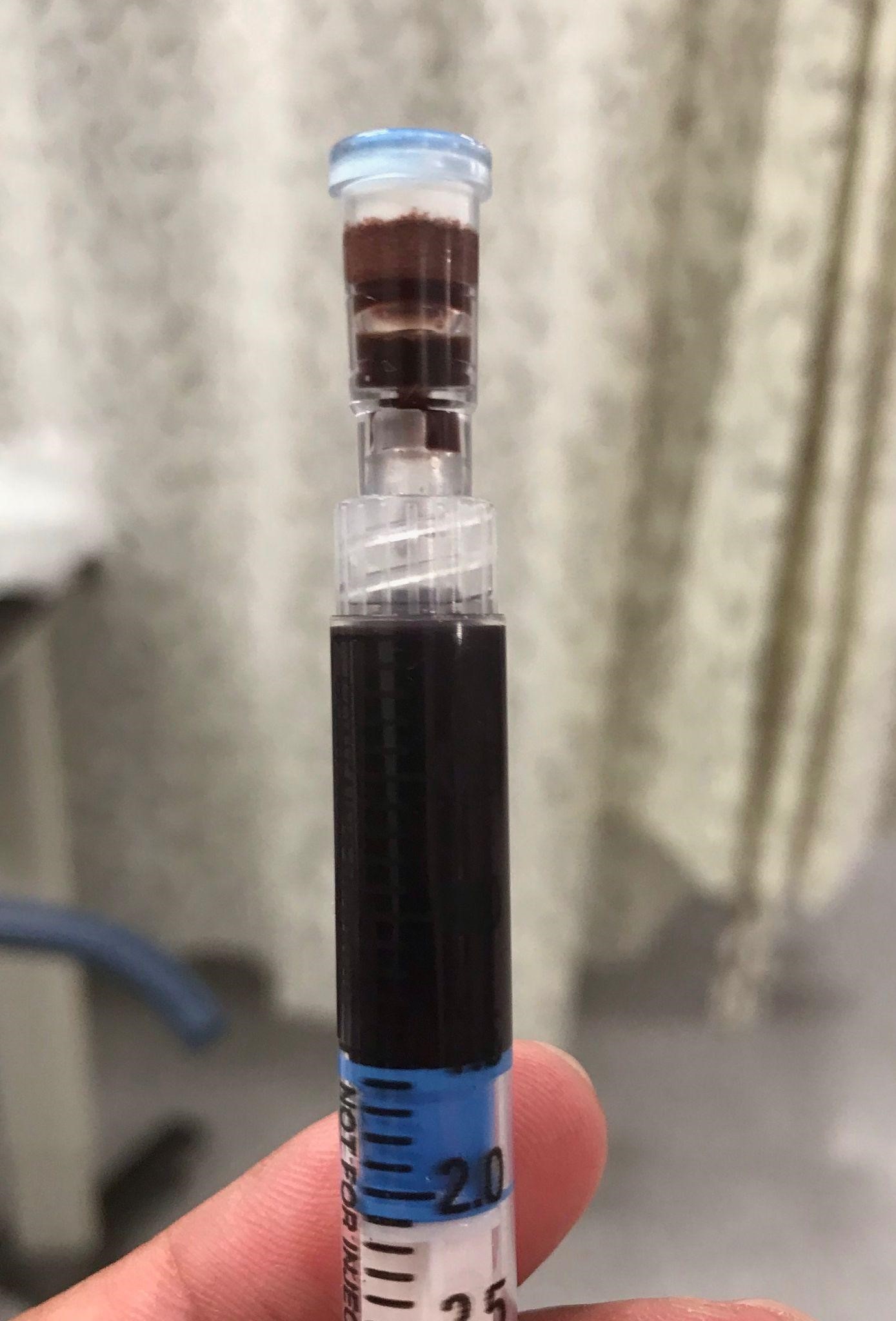
Figure 1. Blood from case patient
Paramedics administer Normal Saline 1L bolus for poor perfusion. Repeat Narcan 2mg IN results in no improvement in mental status or respiratory rate, and she remains hypoxic with an SpO2 of 86% despite high flow oxygen via bag mask ventilation. Given the patient’s persistent ALOC of unknown etiology, paramedics make base contact to discuss the case.
If an ingestion is suspected, identification of the substance while on scene is critical to aiding in the diagnosis at the hospital. Check to see if there are any medications (over the counter, prescription, or unlabeled free tablets) on the patient or in their belongings. Note any drug paraphernalia at the scene including empty bottles or syringes. Medications for medical conditions including narcotics, calcium channel blockers or beta-blockers, psychiatric medications including tricyclic antidepressants (TCAs) are especially important to consider as there are antidotes which may be administered by EMS personnel. Furthermore, if recovered, it is important to bring containers of ingested substances to the receiving hospital for identification and for quantification of ingested dose. Loose tablets/pills may be placed in a plastic bag or container to avoid loss, inadvertent contamination, or further ingestion. Collateral history from bystanders may also yield critical information.
Further history from the patient’s friends elicits that the patient ingested “poppers.” This information is communicated to the Base during Base Contact.
“Poppers” are recreational drugs containing amyl nitrite that are most commonly inhaled, and derive their name from the characteristic ‘popping’ sound made when containers are broken open. They are often bottled in the same style as energy drinks and can carry labels such as “Rush,” “Sub-Zero,” or “Jungle Juice.” They are commonly used by young adults and have the effect of enhancing or prolonging sexual pleasure, inducing euphoria, and creating a general sense of “high.”1

Figure 2. An example of “poppers”
Image Source: https://www.fda.gov/food/alerts-advisories-safety-information/fda-advises-consumers-not-purchase-or-use-nitrite-poppers
Nitrites and nitrates (such as nitroglycerin) are widely used as vasodilators in the treatment of heart failure and ischemic heart disease with the primary purpose dilating large veins. At higher doses, they will also dilate the arteries and can cause hypotension.1 Further, the use of nitrite containing “poppers” can lead to methemoglobinemia.
Methemoglobinemia is a clinical condition defined by a dysfunctional form of hemoglobin that is unable to carry oxygen and offload it to peripheral tissues. It is the result of oxidization of the iron molecules in hemoglobin from the ferrous iron Fe2+ to the ferric ion Fe3+. Nitrites, such as those in “poppers”, have the ability to oxidize iron, resulting in methemoglobinemia. The effect is akin to persons with severe anemia who simply do not have the number of red blood cells or high enough hemoglobin levels to carry oxygen to tissues. For this reason, patients with methemoglobinemia remain hypoxic even with oxygen administration. Many drugs can cause methemoglobinemia as well, including local anesthetics, phenazopyridine (Pyridium), and sulfa drugs. There are also some forms of methemoglobinemia that are genetic such as G6PD enzyme deficiency.
Patients with “popper”-induced methemoglobinemia have symptoms that are related to impaired oxygen delivery including cyanosis. Higher levels of methemoglobin can also result in fatigue, dyspnea, weakness, dizziness, drowsiness, syncope, coma, seizures, and even death.
The Base advises continued high-flow oxygen and ALS transport to the most accessible receiving (MAR). During transport the patient remains hypoxic with SpO2 86% with persistent cyanosis.
For cases of suspected methemoglobinemia EMS should:
- Communicate the suspicion/concern for methemoglobinemia to the Base and/or receiving hospital as this will impact ED treatment.
- Administer high-flow oxygen, and manage the patient’s airway per MCG 1302, Airway Management and Monitoring.
- Administer Normal Saline as needed for poor perfusion.
The patient is transported to the MAR. An arterial blood gas is performed showing a methemoglobin level of > 30% (normal range 0-3%). She is given methylene blue, the antidote for methemoglobinemia, and is admitted to the hospital intensive care unit for further management with subsequent improvement in her clinical status. She is discharged home two days later.
Fun fact, methylene blue can turn bodily secretions, such as urine, blue!
- Base Contact must be made for cases of persistent altered level of consciousness (ALOC) with unknown etiology.
- Abnormal vital signs are a sign of clinical illness; potential underlying causes should be assessed critically and managed accordingly.
- Polysubstance ingestion is common at large festivals, raves, concerts and other events.
- EMS plays a critical role in gathering medications or drugs at the scene in cases of overdose that can provide the clues for ED personnel to the cause of symptoms and guide subsequent treatment.
- Consider methemoglobinemia in patients with persistent low O2 saturations (typically mid-80s) after supplemental oxygen and clear lung sounds.
- Management of patients with methemoglobinemia in the prehospital setting involves supportive care with supplemental oxygen and IV fluids as needed.
References:
- Cole, JB. Cardiovascular Drugs. In Walls, RM. Rosen’s Emergency Medicine: Concepts and Clinical Practice, 9th ed. 2018; p. 1888-1889
- Chandrasekaran E, Erickson T. Poppers, Meet Methylene Blue. EP Monthly. Nov 2014. https://epmonthly.com/article/poppers-meet-methylene-blue/
- https://www.fda.gov/consumers/consumer-updates/nitrite-poppers
Authors: Robert McMickle, MD and Kelsey Wilhelm, MD